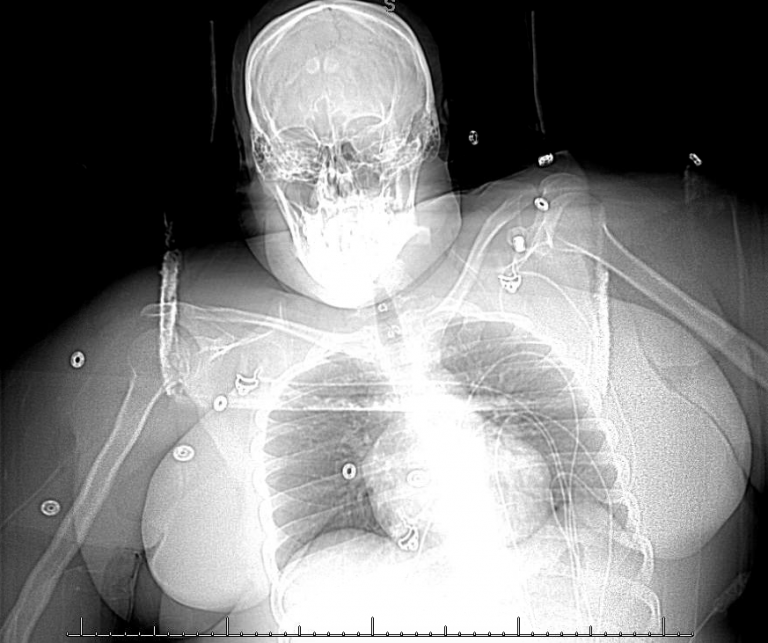
Injection of the right jugular bulb demonstrates a patent right internal jugular vein. It was necessary to demonstrate patency of the right internal jugular vein when planning the stent construct, because the jugular vein would be the distal portion of the outflow tract.
Telescoping stents were placed in the right transverse and sigmoid dural venous sinuses, plastering residual thrombus against the sinus walls and restoring venous outflow. The stents were placed in an overlapping, or telescoping fashion.
The pressure monitoring micro-wire was advanced into the torcula and revealed that once venous outflow was restored the intracranial pressure normalized.